Abstract
Rational: Patients with t-AML are those previously treated for primary malignancy and are categorized with poor prognosis. t-AML treatment options include intensive chemotherapy (IC), hypomethylating agents (HMA) or low dose cytarabine (LDC). However, survival remains poor and allogeneic hematopoietic cell transplantation (Allo-HCT) could lead to better outcomes. The aim of this analysis is to assess the outcome of all consecutive t-AML pts from two regional centers in France, based on treatment intensity, and to identify prognostic factors.
Patients and Methods: between January 2006 and December 2019, 112 adult pts diagnosed with t-AML occurring after treatment of solid tumors (ST; n=72), hematologic malignancies (HM; n=34) or autoimmune diseases (AID; n=6). Pts received chemotherapy and/or radiotherapy or high dose chemotherapy followed by autologous hematopoietic cell transplantation (Auto-HCT) in some. All eligible t-AML pts received intensive chemotherapy (IC, n=55) with the combination of anthracycline and cytarabine in 48 pts and CPX-351 in 7 pts. Unfit pts received non-IC (9 LDC, 24 HMA). The third study group (24 pts) received best supportive care (BSC). Fifteen pts underwent HSCT in first CR.
Statistical analysis: We performed a descriptive analysis of the baseline characteristics and each treatment group was compared with a Kruskal-Wallis test and a Pearson's Chi-square test. Survival curves (Kaplan-Meier method) were compared with a log-rank test. Univariate and multivariate analyses on survival, relapse and NRM were done using Cox regression, Gray test, Fine & Gray regression. The bilateral level of significance was set at 5%. All analyses and graphics were made under the R program (v3.5.1). A pair-matched control analysis with de novo AML was performed only on pts who received IC matched for age, cytogenetics and ELN 2010 classification.
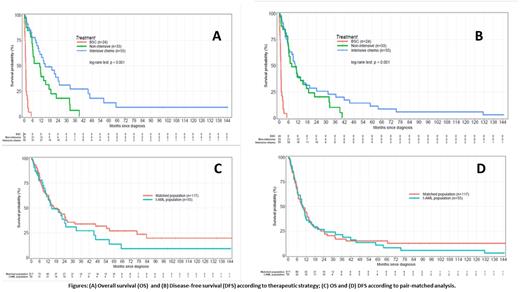
Results: A total of 112 t-AML pts were identified, 56 were males (50%) with a median age of 68 yrs (19-87) at t-AML diagnosis. Before t-AML, 72 pts had ST (64.5%), 34 HM (30.5%) and 6 AID (5%). Forty-six pts (41%) received chemotherapy alone for their primary cancer, 17 (15%) radiotherapy alone, 49 (44%) radio chemotherapy, 17 (15%) auto-HCT and 6 (5%) long-term methotrexate for AID. Median interval from treatment of previous ST or HM to t-AML diagnosis was 4.7 years in ST, 6.6 years in HM and 21 years in AID (p=0.03). At t-AML diagnosis, 42% of pts presented an unfavorable karyotype and 44% an unfavorable ELN 2010 classification. Regarding molecular alterations, FLT3-ITD, FLT3-TKD, NPM1 and IDH1/2 mutations were observed in 6.9, 2.3, 11.5 and 2.3% of pts respectively. MECOM1 was overexpressed in 25.5% of cases. Among treated pts (n=88), 43 pts (49%) achieved CR: 4 from 33 (12%) in non-IC pts (3 in HMA and 1 in LDC) and 39 from 55 (71%) in IC pts. Fifteen pts (17%) underwent Allo-HCT with a median interval between AML diagnosis and Allo-HCT of 4.7 mo (2.6-17.5). The best response after transplantation was CR in 10 pts; at the last follow up, 4 pts are alive (3 in CR and 1 in relapse) and 11 died (5 from relapse, 5 from TRM causes and 1 from another subsequent malignancy). Overall, with a median follow up of 5.5 mo (0-144), the median OS and DFS were 9 mo (5.9-13.5) and 6.3 mo (5.3-10.3) respectively (Figure). There was a significant difference between the 3 treatment groups concerning OS (p<0.001) and DFS (p<0.001) with a significant difference in OS between IC and non-IC groups (p=0.02). In the 88 treated t-AML pts, with a median follow up of 8.2 mo (0.3-144), the median OS was 13.5 mo (10.3-19.6) and the median DFS was 8.2 mo (7-13.7). Multivariate analysis for total and treated populations showed no impact of all variables related to previous malignancies except for auto-HCT pre-t-AML (significant negative impact on OS, DFS, NRM), WBC at t-AML diagnosis (negative impact on OS, DFS) and chemotherapy (positive in total population on OS, DFS, NRM and negative impact of IC on OS and NRM in treated pts) . In IC treated pts, we showed, in a pair-matched analysis with de novo AML, no difference in term of OS and DFS due to a significant higher CI of NRM (p=0.045) at 24 mo (40% in t-AML versus 27.4% for de novo AML) and a lower CI of relapse (NS) at 24 mo (33% in t-AML versus 47.6% for de novo AML).
Conclusion: The prognosis of t-AML remains poor and our study showed the advantage of using intensive chemotherapy whenever possible and, in comparison with de-novo AML, a higher NRM and a lower incidence relapse.
Nicolini: Sun Pharma Ltd.: Consultancy, Membership on an entity's Board of Directors or advisory committees; Kartos Therapeutics: Consultancy, Membership on an entity's Board of Directors or advisory committees; Novartis: Honoraria, Membership on an entity's Board of Directors or advisory committees, Other: travel, accommodations, expenses, Research Funding; Incyte Biosciences: Honoraria, Other: travel, accommodations, expenses, Research Funding, Speakers Bureau; BMS: Honoraria.